Cuidados paliativos y políticas de drogas: el choque de dos mundos
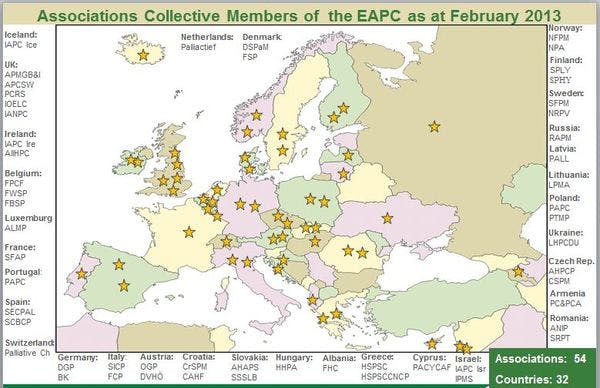
En el congreso internacional de la Asociación Europea de Cuidados Paliativos (EAPC), médicos y proveedores de atención de la salud pública discutieron los obstáculos para acceder a medicamentos opioides y el derecho internacional relacionado con este derecho humano. Más información, en inglés, está disponible abajo.
Suscríbase a las Alertas mensuales del IDPC para recibir información sobre cuestiones relacionadas con políticas sobre drogas.
Plenary sessions and side meetings at the recent European Association of Palliative Care (EAPC) World Congress in Prague focused on promoting palliative care as a human right. This meant that several sessions discussed barriers to access to opioid medicines – and particularly the international laws that restrict access on the one hand, and guarantee human rights on the other. Nearly three quarters of the world’s population live in countries where medical opioid consumption is near to zero. At the same time, just over one-fifth of the world’s population consume 93.8 percent of all licitly produced morphine.
A detailed analysis of current global consumption levels versus projected needs (by former WHO essential medicines expert Dr Willem Scholten) raised the question of whether global production will ever be able to keep pace with medical demand. Current production of opioid medicines is 290 tonnes, or one-fifth of the estimated need to address pain globally. Adequacy would require production to increase to 1,448 tonnes of morphine equivalent. As a result, new areas of legal poppy production and laboratories for synthetic opioid manufacture should be created to meet the global need for these medicines.
The global pandemic of untreated pain is caused by domestic over-regulation of narcotic drugs beyond the requirements of the UN drug conventions – driven by a sense of “opioidophobia”. Medical providers are untrained in the use of controlled narcotics, and many are constrained by fears of criminal prosecution. Many providers view this endemic under-treatment as an ethical and human rights issue – one that should be raised in national and international policy forums and seen as a violation of UN covenants requiring countries to provide the “highest attainable standard of health”. The Executive Board of the World Health Assembly will be considering a proposal at its 2014 meeting to declare access to palliative care a human right. In the meantime, the European Association of Palliative Care has launched the “Prague Charter” which inscribes these principles and demands.
One of the great things about participating in a Congress such as the EAPC was being surrounded by colleagues who care so passionately about their profession and about their patients, families and communities. I had a similar feeling at this year’s Commission on Narcotic Drugs (CND) in Vienna, spending a week with colleagues whose dedication to changing drug policy was inspiring. Similarly, I look forward to spending this week at the international harm reduction conference in Vilnius with colleagues from the worlds of public health, human rights and drug policy. If we all put our heads and hearts together, the combined power and brilliance would be an irresistible force for change.
For more information visit: Report of the European Association of Palliative Care international congress in Prague 2013.
Keep up-to-date with drug policy developments by subscribing to the IDPC Monthly Alert.
Temas
Perfiles relacionados
- European Association of Palliative Care